-
Foods that Affect Sperm Count

Did you know that the sperm count of the average man has steadily decreased over the past 40 years? Why is this happening? Is it a problem that the quality of sperm is decreasing? It is certainly a problem for a man who is struggling with infertility. Fortunately, there are some things you can do to promote your sperm quality, and it starts with eating the right foods.
How big of a problem is decreasing sperm quality? The Centers for Disease Control and Prevention (CDC) estimates that a male factor as well as a female factor is involved in about 35 percent of couples experiencing infertility. Additionally, a recent study estimates that sperm counts have dropped by 59 percent, on average over the past 38 years. What’s causing this decrease? No one really knows. Some blame technology like cell phones and laptops, which produce fertility-threatening heat. Obesity may be a factor. And there’s a body of research to indicate that a man’s diet has an impact on sperm count. Here are the dietary do’s and don’ts for improving your fertility.
First, here are the foods to avoid if you want to boost fertility:
- Processed meats, eaten three or more times a week, can reduce your chance of achieving pregnancy by 28 percent. Red meat is also related to low sperm concentration and sperm count, and processed red meat also alters sperm motility. Eating fish and poultry is better for your fertility.
- Trans fats increase the risk of heart disease and decrease sperm counts. In fact, sperm with the highest trans-fatty acid levels are linked to low sperm concentrations. Trans fatty acids typically come from French fries and commercially baked items, as well as foods like frostings and things cooked with lard.
- Soy products have phytoestrogens, estrogen-like compounds that interfere with fertility. Soy milk, veggie burgers, protein bars, tofu, and tempeh are soy-based foods linked to low sperm count, particularly in overweight men.
- High fat dairy products have been linked to abnormal sperm shape and low motility. Whole milk, cheese, and cream are all on the do-not-eat list, because as few as three slices of cheese a day can endanger fertility. Low-fat dairy, however, is linked to higher sperm concentration and motility.
- Pesticides and bisphenol a (BPA) can make their way into your food and diminish fertility. Pesticides can be on vegetables and fruits as well as meat and fish. BPA is in food packaging and cans and can leech into the foods we eat. These chemicals, which area also found in non-stick cookware act as xenoestrogens and decrease sperm concentration.
- Sometimes what you drink can impact your fertility. Alcohol and beverages with excessive caffeine have been linked to a decrease in male fertility.
Now that you know what to avoid, what should you eat? Certain foods have been shown to increase male fertility and improve sperm health.
- Eat your veggies. Fruits and vegetables, especially green leafy vegetables and legumes, have been shown to improve sperm concentration and motility. It’s believed that this is due to the high level of antioxidants and nutrients like co-enzyme Q10, vitamin C, and lycopene, micronutrients linked to higher sperm concentration.
- Have some fish or chicken. Research indicates that eating chicken and fish can actually improve fertility. Fish rich in omega-3 fatty acids, in particular, raise sperm count significantly. On the other hand, taking omega 3 supplements does not have the same effect.
- Walnuts can give your fertility a boost. In a small 2012 study, significant improvements in sperm vitality were seen with the consumption of only 18 walnuts a day.
At the Center for Vasectomy Reversal, we love helping people start families with healthy pregnancies. We pride ourselves on helping men improve their fertility through uncompromising, concierge-level patient care. Under the direction of Dr. Joshua Green, our team provides state-of-the-art treatment for men who need a reversal of their vasectomy or have other fertility concerns. To learn more, contact us through our website or call 941-894-6428.
-
How Stress Affects Semen Quality

It’s long been understood that stress has an impact on a person’s health, so it comes as no surprise to learn that men’s reproductive health may be affected by stress. About 12 in every 100 couples in the United States struggles with infertility, and several studies over the past several years have established a link between poor semen quality and stress. Now, a new study is taking a closer look at both subjective and objective measures of stress to try to determine how it’s connected with semen concentration and sperm motility and appearance.
Male infertility is the problem for about 40 percent of couples with fertility issues. The main cause of male infertility is sperm abnormality, including misshapen or immobile sperm or low sperm production. Sometimes, these abnormalities are caused by medical conditions, but they can also be caused by health and lifestyle factors.
The new study, published in the journal Fertility and Sterility was conducted by researchers from the Rutgers School of Public Health in Piscataway, NJ and Columbia University’s Mailman School of Public Health in New York, NY. Between 2005 and 2008, researchers looked at 193 men between the ages of 38 to 49 who were a part of the Study of the Environment and Reproduction at the Kaiser Foundation Health Plan in Oakland, CA. The men completed a series of tests to measure stress levels, including workplace stress, stressful life events, and perceived stress. They also provided sperm samples, which were analyzed for semen concentration, sperm shape, and sperm movement (motility).
According to the researchers, men who felt stressed had lower concentrations of sperm and more sperm that were misshapen or had impaired motility. Even after considering other factors, like a history of reproductive health or other health problems, life stress negatively impacted sperm quality. Interestingly, job stress did not have the same effect. However, men with stressful jobs had lower levels of testosterone, and unemployed men had a lower quality of sperm than even stressed-out men with jobs.
The researchers don’t fully understand how stress affects semen quality, but they have some theories. It could be that stress triggers the release of glucocorticoids, steroid hormones which lower testosterone and dampen sperm production. Oxidative stress could also be a factor because oxidative stress in the body can degrade semen quality.
What is known is that a man can improve his fertility, even under stress, with healthy lifestyle habits. Staying physically active and practicing stress-reducing relaxation techniques can help, as can eating a nutritious diet and maintaining a healthy BMI. Men who are trying to improve their fertility should quit smoking, limit alcohol consumption, and talk to a doctor before beginning any new medication.
At the Center for Vasectomy Reversal, we pride ourselves on helping men improve their fertility through uncompromising, concierge-level patient care. Under the direction of Dr. Joshua Green, our team provides state-of-the-art treatment for men who need a reversal of their vasectomy or have other fertility concerns. To learn more, contact us through our website or call 941-894-6428.
-
What are Anti-Sperm Antibodies?

Are you and your partner struggling to become pregnant following vasectomy reversal surgery? Many factors affect the success rate of this procedure, including the potential development of anti-sperm antibodies. While this is a less common cause of male infertility, it’s still a factor worth exploring.
What are Anti-Sperm Antibodies?
Under normal conditions, sperm only exists within a man’s closed reproductive system. The tubules through which sperm travel don’t mix with other parts of the body. However, if sperm enters the bloodstream for any reason, the body’s immune system perceives the sperm as a foreign protein and produces anti-sperm antibodies in response.
Anti-sperm antibodies may cause sperm to clump together, reducing their ability to swim and subsequently reach the female egg. In rare cases, the antibodies can also cover the head of the sperm, rendering them unable to penetrate and fertilize the egg.
What Causes Anti-Sperm Antibodies?
In short, any time semen mixes with blood inside the body, anti-sperm antibodies are liable to form. Men may develop these antibodies for any of the following reasons:
- Vasectomy or other testicle surgery
- Tramatic testicle injury
- Prostate infection
Women’s reproductive systems can also produce anti-sperm antibodies if they have an allergic reaction to their partner’s semen. If present in the cervical mucus, these antibodies could damage or kill sperm as they enter the vagina. This condition is rare and not fully understood by the medical community.
Testing for Anti-Sperm Antibodies
An immunobead test (IBT) detects the presence of sperm-destroying antibodies in the blood, seminal fluid, or cervical mucus. Testing also indicates what part of the sperm is specifically affected. When performed on blood, an IBT can reveal whether the anti-sperm antibodies originate from the patient’s blood or reproductive system.
Because anti-sperm antibodies are relatively rare, and their presence doesn’t always cause infertility, your physician will likely review your medical history and conduct other tests before suggesting an IBT. Anti-sperm antibody testing should only be necessary if another cause of infertility can’t be found or the results of routine testing are inconclusive.
Treating Anti-Sperm Antibodies
While high levels of anti-sperm antibodies can make it difficult for some couples to get pregnant, their presence does not guarantee fertility issues. In fact, some findings suggest a low correlation between anti-sperm antibodies and the ability to conceive.
Still, if you’re having trouble getting pregnant, you may choose to pursue treatment for anti-sperm antibodies. Your options include immune response-lowering medication and assisted reproductive technology (ART), such as intrauterine insemination.
Dr. Joshua Green of the Center for Vasectomy Reversal is a leader in helping men overcome infertility problems. All infertility procedures we offer, including vasectomy reversal, are performed by a qualified surgeon using state-of-the-art equipment. Patients can expect concierge-level care and friendly staff interactions all along the way. To discuss your fertility concerns with Dr. Green, please contact our Sarasota, FL clinic at 941-894-6428 or schedule a free consultation online.
-
Semen Analysis Testing After a Reversal
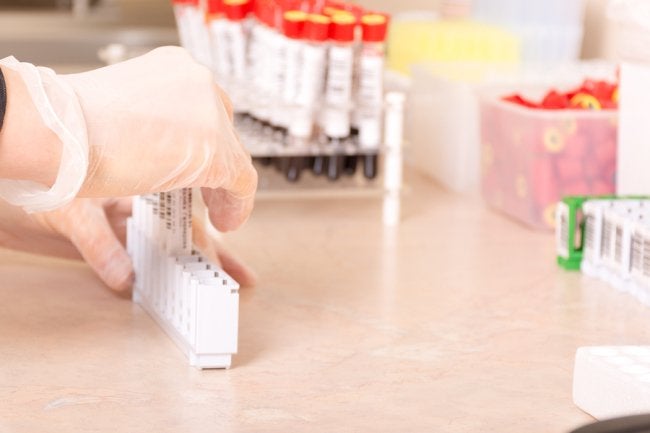
Vasectomy reversals have favorable success rates, but there’s still a waiting period before couples are able to get pregnant. Every couple is a little different, but in general, it may take anywhere from three to 12 months before a man’s sperm count is once again at a robust level. To assess the success of the vasectomy reversal, men will have semen analysis testing.
Depending on the particular clinic, men may have their first analysis at about six to eight weeks after the procedure. After this, additional semen analysis appointments are scheduled every one to two months. Once a lab report shows stabilized sperm count and motility, there is a good chance of pregnancy within six months of actively trying.
At the Center for Vasectomy Reversal, Dr. Joshua Green can answer all of your questions about having a vasectomy reversal in Sarasota, including what you can expect afterward. If you’ve decided your vasectomy wasn’t the right decision for you, give us a call at (941) 894-6428.
-
What Men Should Know About Semen Analysis
A doctor may request a semen analysis after a man undergoes a vasectomy or a vasectomy reversal, or if a couple has been having unprotected sex for six to 12 months, yet hasn’t been able to conceive a child. When a semen analysis is performed after a vasectomy, it is for the purpose of confirming that there is no sperm present in the semen. After a vasectomy reversal, a semen analysis is used to evaluate the success of the procedure.
You can hear more about semen analysis by watching this video. It explains that the lab technician will check the semen sample for semen volume, semen thickness, sperm count, sperm motility, and sperm morphology. All of these factors affect fertility.
If you and your partner haven’t been able to conceive a child because of a prior vasectomy, make an appointment to see Dr. Green at the Center for Vasectomy Reversal. Call (941) 894-6428.
-
What You Need to Know About Semen Analysis
If you’ve undergone a vasectomy, you’re probably already familiar with the basic procedure of semen analysis. Physicians commonly request a semen analysis after a vasectomy to ensure that there is no sperm present in the semen. However, this series of tests is also helpful for men who have undergone vasectomy reversals. In these cases, semen analysis after the procedure can evaluate its success.
You can hear more about semen analysis by watching this animation. It explains that men may provide a semen sample in a sterile medical cup or a special condom. If men collect the semen sample at home, they must keep it at body temperature and take it to the lab or doctor’s office within two hours. This video also discusses the various aspects of semen and sperm that the tests will evaluate.
Dr. Joshua Green in Sarasota has helped countless men achieve their dreams of becoming fathers through vasectomy reversals. Call the Center for Vasectomy Reversal at (941) 961-4581 to schedule a consultation with Dr. Green.
Recent Posts
Popular Posts
categories
- Uncategorized
- Sperm Retrieval
- vasectomy reversal
- Emergency
- Dr. Green
- sperm count
- fertility
- male infertility
- MESA
- medical care
- low sperm count
- IVF
- male fertility testing
- anesthesia
- pregnancy
- sperm aspiration
- semen analysis
- post-vasectomy pain syndrome
- infertility
- VE
- anti-sperm antibodies
- older dad
- general anesthesia
- gender reveal party
- post-operative infections
- baby name
- parent
- baby's first year
- fertilization process
- spinal anesthesia
- ACS Fellow
- nutrition tips
- concierge-level care
- fertility planning app
- azoospermia
- out-of-town patients
- V-V
- post-vasectomy reversal
- conceiving
- vasectomy
- vasoepididymostomy
- smoking
- sperm quality
- baby registry
- infographic
- surgical care
- surgical consultation process
- prostate cancer
- baby gender
- family time
- COVID
- Baby Shower
- Child Care
- Halloween Costume Ideas for Babies
- Halloween
- Halloween Safety Tips
- Celebrity Infertility Spotlight
- Postpartum
- testosterone
- Father's Day
- Father
- Men's Health
- Thanksgiving
- Pregnancy Announcement
- Parenting Tips
- Sperm
