-
Understanding Male Fertility: Common Misconceptions and What You Should Know

Infertility is a common problem, impacting about 15 percent of all couples. If you are struggling with infertility, it is important to have all the facts, but there are many misconceptions that still exist regarding male fertility. Here, we look at some myths about infertility, as well as offering some hope to men who are facing this problem. Continue reading “Understanding Male Fertility: Common Misconceptions and What You Should Know”
-
Can Coffee Affect Sperm Health?

In the pursuit of parenthood, you’re doing all you can to facilitate the plan. Are there roadblocks in your way that you may not even know about? What foods can you eat to ensure a healthy sperm count? What foods should you cut out? What about coffee? Is it dangerous to sperm? Here’s everything you need to know about coffee and how it affects sperm health.
The Fertility Journey
As we embark on the path to better fertility in the pursuit of parenthood, it is evident that both the carrier of the child and the provider of the sperm will need to make a few lifestyle changes. Some of these changes can include:- Getting More Rest
- Cessation from Smoking
- Limiting or Quitting Alcohol Consumption
- Getting More Exercise
We also know that someone carrying a child should limit coffee intake. Excessive coffee intake has been linked to several complications during fertility and pregnancy, including premature birth, pregnancy loss, and fetal growth issues.
Coffee’s Effect on Sperm Health
There is substantial evidence that the quality of semen has declined worldwide. Is coffee to blame? Multiple studies have been conducted to study the effects of coffee on sperm, and here are the most recent findings.- Coffee Doesn’t Affect Sperm Count
Currently, no studies show that coffee’s caffeine intake affects sperm count. Cola drinkers did have a lower sperm count, but they also had other poor nutritional habits that may have contributed to these effects. - Coffee Doesn’t Affect Sperm Concentration
A recent study showed that men who consume four or more cups of coffee daily have a higher sperm concentration than men who drink 0 cups of coffee per day. However, men who consume 1-3 cups of coffee daily have the highest sperm concentration of these three groups. - Coffee Does Seem to Alter DNA of Sperm
Some studies have shown that coffee intake is related to damaged or altered DNA, specifically double-strand DNA breakage. - Coffee Intake Does Seem to Increase the Time it Takes to Conceive
There is also corelative evidence that links coffee intake with lengthening the time it takes to conceive.
Conclusion
Caffeine intake from coffee does not seem to have a significant effect on sperm count or concentration, but there does seem to be some DNA damage that is related to coffee intake. Additionally, caffeine intake from cola did have a slightly negative effect on sperm count and quality. A recent study concluded that those who consumed a moderate amount of coffee had a higher likelihood of conceiving than those who drank a low amount. The same study concluded that high levels of coffee consumption had adverse effects. Consuming caffeine from any source in moderation is likely the best choice while trying to conceive.Center for Vasectomy Reversal
If you are considering a vasectomy reversal, it’s essential to understand everything that goes into the procedure. The Center for Vasectomy Reversal can help. Read our patient reviews to learn about our increasingly positive satisfaction rate. We will help you navigate the challenges on the way to becoming a parent. When you’re ready to check us out, visit our website or call us at (941) 313-7749. -
Unlocking Fertility Secrets: How Lifestyle Impacts Your Reproductive Health

How Lifestyle Impacts Your Reproductive Health.
Optimizing Fertility through Lifestyle
If you have been trying to conceive without success, consider this: when it comes to fertility, lifestyle factors can have a major impact. There are some elements of fertility that are beyond your control, of course, like your genetic makeup and your age. However, there is a lifestyle and infertility connection to indicate that changing your habits may be helpful in improving your chances of conception. Here, we offer some suggestions for adopting healthy habits for fertility.
Improve Your Diet, Improve Your Fertility
When you eat a nutrient-dense diet, filling your plate whole grains, healthy fats, lean proteins, and plenty of multi-colored fruits and vegetables, you are doing something that supports both male and female fertility, benefiting sperm production and ovulation alike. Consuming essential nutrients like folic acid, iron, zinc, and antioxidants can protect the body from inflammation and cellular damage, and help promote a healthy pregnancy. Trans fats should be limited or avoided entirely, as they are linked with higher risks of infertility. Strive to maintain a healthy weight, as being underweight or overweight can impede fertility.
The Right Amount of Exercise Can Improve Fertility
Regular moderate to vigorous exercise is good for the fertility of men and women alike. Strive for physical activities that elevate your heart rate, like brisk walking, because this kind of activity is linked to higher-quality sperm and better maternal and fetal health outcomes. It is important for women to avoid workouts that are too intense, though. While exercising in moderation promotes reproductive and overall health, excessive exercise can inhibit ovulation and disrupt a woman’s hormonal balance, decreasing a woman’s chances of conceiving. A sedentary lifestyle is just as bad for a person’s health, and can lead to obesity, which can diminish fertility. According to the American College of Obstetricians and Gynecologists, women should be encouraged to participate in aerobic and strength conditioning exercise before, during, and after pregnancy. Finding the right balance can be tricky, so if you have concerns, speak to your doctor.
Reducing Your Stress Can Benefit Your Reproductive Health
Stress, on its own, does not cause infertility. However, it is one piece of the puzzle, and there is evidence to suggest that people with a long history of anxiety or depression may have trouble conceiving, both naturally and with IVF. This issue needs to be studied further, but it does help to try and manage your stress when trying to conceive. Of course, properly managing your stress is important for your overall health, as well.
The Reproductive Health Impact of Substance Use
As is evidenced by the impact of dietary options on your fertility, what you put into your body matters. Women have long been told to completely avoid alcohol when trying to conceive, and there is evidence to indicate that consuming alcohol when attempting IVF lowers the chance of conception by as much as 16 percent. However, what is less well known is that men should avoid alcohol when trying to conceive, as well. Excessive alcohol consumption has been linked to reduced testosterone levels, and can also make it difficult to maintain an erection.
Cigarette smoking also reduces fertility in both men and women. If you needed another reason to quit smoking, in addition to the long list of reasons that already exist in regard to your overall health, smoking damages eggs and sperm, decreases motility, is harmful to the lining of the uterus, damages DNA, and impedes essential hormone production. Quitting smoking should be high on your list of lifestyle changes if you are trying to conceive.
This may not even need to be said, but illicit drug use is not something you should be participating in when trying to conceive. Drugs like marijuana, cocaine, LSD, ecstasy, and methamphetamines can disrupt menstrual cycles as well as lowering sperm count, testosterone levels, and total seminal fluid. For the sake of your fertility, and for many other reasons, recreational drugs should be avoided, particularly when trying to conceive.
Center for Vasectomy Reversal Cares About Men’s Health
When you are trying to achieve pregnancy, it is important to understand the impact your lifestyle choices have on your reproductive health. Of course, it is also vital that you partner with healthcare providers who can help you improve your reproductive and overall health. At the Center for Vasectomy Reversal, men’s health is our priority. We pride ourselves on helping men improve their health and fertility through uncompromising, concierge-level patient care. Dr. Green and his team provide state-of-the-art treatment for men who need a reversal of their vasectomy or have other fertility concerns. Having had extensive training in urology, microsurgery, and vasectomy reversal, Dr. Green founded the Center for Vasectomy Reversal to provide the highest level of patient care while delivering optimal surgical results. To learn more about how our experienced team can help you reach your reproductive goals, contact us through our website or call 941-894-6428.
-
Preserving Fertility: A Deep Dive into Modern Methods
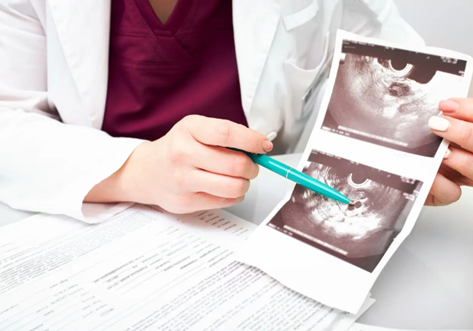
Reproductive Health Innovations
If you are struggling with infertility, working with a specialist can help you determine which treatments are right for you. As science progresses, more and more treatments are available, both in terms of achieving pregnancy and fertility preservation options. Both male and female infertility issues can be overcome with the correct strategies when you work with an experienced reproductive specialist. Here, we look at some modern IVF techniques, along with other treatments available to overcome infertility.
Overcoming Obstacles to Fertility
Certain physical barriers to fertility can be treated by specialists, like a blocked fallopian tube. Tubal blockage is overcome using IVF, which allows fertility specialists to retrieve eggs without the help of the fallopian tubes, allowing fertilization to occur. This is not the only way to deal with blocked fallopian tubes, as there are also medications that can encourage ovulation if only one side is blocked, and procedures that can help unblock a tube. There is also medication to help overcome male infertility, and ICSI allows sperm to be directly introduced into an egg, for higher success rates with in vitro fertilization.
Pre-Implantation Genetic Screening
One of the most amazing advances in modern fertility treatment is the ability to genetically test embryos before attempting to transfer them into the uterus. Preimplantation genetic testing allows doctors to choose a genetically healthy embryo to transfer, reducing the rate of failed embryo transfers and miscarriages. This also reduces the risk of multiple pregnancies, because the fertility specialist can find the correct embryo to transfer, rather than transferring several at once in the hope of successful implantation. Preimplantation screening also helps detect genetic disorders and reduce the risk of birth defects.
Vitrification
This fast freezing method is used to cryopreserve embryos and eggs, so that they can be preserved for years in glass-like structures. This is one of the most popular fertility preservation techniques available, allowing women to postpone pregnancy when battling cancer or for some other reason. Sometimes young women want social egg freezing, so that they can delay pregnancy until they are financially stable and emotionally able to raise a child. When compared to the older slow freezing method, vitrification has doubled pregnancy rates. It helps women receiving fertility treatments to avoid ovarian hyperstimulation syndrome, and enables preimplantation genetic screening.
Ovarian Tissue Freezing
Sometimes, especially for women and girls facing cancer treatments or undergoing gender affirmation surgery, ovarian tissue freezing is the best option for preserving future fertility and hormone production. In this procedure, the egg-producing portion of the ovary is removed, frozen, and stored, until years later, when it can be transplanted to make pregnancy possible or resume natural hormone production. Ovarian cryopreservation success rates are at about 30 percent right now, and as technology leads to improved methodology, that rate is expected to increase.
Freeze-all strategy
This approach is a combination of IVF, vitrification and preimplantation genetic testing, in which healthy embryos are frozen to be implanted at a later date. This way, patients can us the frozen embryos when they are ready to resume IVF treatment. This avoids the risk of hyperstimulation from fertility drugs and hormones, by allowing the woman to take a break from fertility treatment for a time. It also allows the fertility specialist to help correct hormone levels that may not be conducive to a successful pregnancy. Once the hormones are in balance, the embryo can be transferred.
Center for Vasectomy Reversal Cares About Men’s Health
All of these advances in fertility preservation are very exciting, and the best way to assure your best chance at conceiving is to work with experienced fertility specialists who care about the health of everyone involved in the pregnancy. At the Center for Vasectomy Reversal, men’s health is our priority. We pride ourselves on helping men improve their health and fertility through uncompromising, concierge-level patient care. Dr. Green and his team provide state-of-the-art treatment for men who need a reversal of their vasectomy or have other fertility concerns. Having had extensive training in urology, microsurgery, and vasectomy reversal, Dr. Green founded the Center for Vasectomy Reversal to provide the highest level of patient care while delivering optimal surgical results. To learn more about how our experienced team can help you reach your reproductive goals, contact us through our website or call 941-894-6428.
-
Can Certain Medications Affect Your Sperm Health?

Man rethinking taking medication.
Often, infertility is assumed to be a woman’s problem. However, male infertility is also significant, and sperm quality can heavily impact the chances of conception. Many factors can affect male fertility, including excess weight, cigarette smoking, excessive drinking, and use of recreational drugs. While all of these factors are commonly known, what is less well known is that certain medication can interfere with male fertility.
How can medications affect a man’s fertility? Often, medication will decrease the production of sperm, but in some cases, medications will affect the function of the sperm itself. Decreased production leads to low sperm count, which means fewer sperm will be available to fertilize an egg. If a medication impacts the motility of the sperm, that means the sperm won’t move as efficiently and will have difficulty reaching the egg. Generally, once a man stops taking medication, it takes at least two or three months for his sperm to recover, since it takes that long for sperm to form and mature. With certain medications, however, it can take months or years for fertility to return to normal, and it might not return at all.
So, what types of medications have a negative impact on sperm? Over-the-counter medication does not usually cause an issue, as long as it’s taken correctly and in the proper dosage. However, it’s important to be cautious when you’re trying to conceive, so it’s wise to discuss any OTC medications with your doctor. Certain OTC medicines warrant particular caution:
- Non-steroidal anti-inflammatory drugs (NSAIDs) sometimes reduce fertility. According to a recent study, men taking 1,200 mg of ibuprofen daily can develop a hormonal condition that causes a problem, especially if the man is older. What was not made clear in the study is whether lower doses of ibuprofen can have the same effect. Additionally, while the effects are reversible when the medication is taken for short periods of time, it’s unclear whether they’re reversible if taken long-term.
- Natural or herbal remedies can cause problems for men trying to conceive. Because herbal remedies are not held to the same regulatory standards as medications, it’s better to stay away from them to protect fertility. Supplements that contain testosterone can be particularly problematic, so avoid anything that uses terms like “male enhancement,” “andro booster,” or “T-booster.”
There are prescription medications that can have a significant impact on fertility.
- Steroids and testosterone therapy can have a strong negative impact on sperm production. In fact, testosterone supplements will completely stop sperm production. Whether the man is taking anabolic steroids, herbal supplements with testosterone, or a prescription testosterone replacement from the doctor, the effect is the same. Testosterone blocks the body’s natural hormonal signals that cause the testicles to make sperm. The result is that the semen will either have a very low concentration of sperm or will have no sperm at all. This effect is reversible, but it takes a long time for the sperm to recover. In fact, it can take six to 12 months for sperm count to get back to normal.
- Chemotherapy can wipe out your sperm count. This is because chemo works by killing rapidly dividing cells, like cancer cells, but also, unfortunately, sperm cells. After cancer treatment, it’s common for men to have no sperm in the semen. However, natural fertility can return one to five years after the treatment is discontinued. If you’ve been through chemo, it’s best to wait at least two years before attempting to conceive. For some people, though, fertility never recovers. If you are about to start chemotherapy, talk to your doctor about freezing your sperm for later use.
- Blood pressure medications can decrease semen volume, sperm concentration, and sperm motility. These medications, especially calcium channel blockers, can also cause decreased libido and erectile dysfunction.
- Opioids can interfere with sexual performance and fertility. Long-term use, in particular, can disrupt the signals that control testosterone production. If you’ve only used opioids short-term, as for the treatment of a broken bone or when recovering from surgery, you may not need to worry.
- Antidepressants can cause a drop in libido and may negatively affect sperm production. Selective serotonin re-uptake inhibitors (SSRIs) are the most common medications used to treat depression and anxiety, and they can hinder your chances of conception. However, there are other medications your doctor or mental health provider can prescribe that won’t have the same impact.
- Other medications may be problematic if you’re trying to conceive. Antibiotics can interfere with testosterone and sperm production, especially an antifungal antibiotic called Ketoconazole. Biologics, used to treat autoimmune disorders, can reduce sperm count, and alpha-blockers, prescribed to treat the symptoms caused by an enlarged prostate, can inhibit ejaculation. 5-alpha-reductase inhibitors like Propecia® and Avodart®, used for hair loss and prostate enlargement treatment, can make it hard to conceive, but the effect goes away when you stop taking them. Anti-epilepsy medications, antiretrovirals, blood pressure medications, and some other medications can also cause fertility problems.
At the Center for Vasectomy Reversal, we are concerned with every aspect of men’s health, and we pride ourselves on helping men improve their fertility through uncompromising, concierge-level patient care. Under the direction of Dr. Joshua Green, our team provides state-of-the-art treatment for men who need a reversal of their vasectomy or have other fertility concerns. To learn more, contact us through our website or call 941-894-6428.
-
What are ovulation cycles and do you need to consider that when trying to conceive?

When you’re trying to conceive, you’ll learn a lot of information that may feel confusing. One of the most important things to understand during this time, though, is the ovulation cycle. There’s a very small window within this cycle when it’s possible to conceive, so knowing when that window occurs is crucial to your success. While ovulation can seem mysterious, especially to a person who doesn’t menstruate, it’s actually fairly simple science. Here’s what you need to know.
First, let’s talk about the amazing fact that women are born with one to two million eggs in their bodies. Of course, they only release 300 to 400 of those in a lifetime, but it’s still very interesting. Eggs are generally released one at a time, once a month, and each egg is available for fertilization for about 24 hours before it dissolves. That’s a pretty short window! Even when you consider the fact that sperm can hang around for about three to five days in order to meet up with the egg, it’s pretty miraculous that conception ever occurs at all. It’s easy to see, though, why timing is everything.
Ovulation happens somewhere between day 11 and day 21 of a woman’s cycle, but how do you know when it’s happening? If a woman has a very regular, 28 day cycle, you can count 14 days back from when the next period is going to start, and plan to have sex every other day right around that time. It might seem counterintuitive to skip days, but the fact is that a man’s sperm count can be lowered by having daily sex.
What if your partner doesn’t have a regular cycle? Cycles can vary widely, ranging from 23 to 35 days, and even within a cycle, the time of ovulation isn’t always the same. The best way to determine if ovulation is happening is by tracking it through a few different methods.
- Pay attention to bodily clues. Cervical mucus starts resembling egg whites, the senses of smell and taste may be heightened, breasts may become tender, and she may experience mild abdominal pain. In some women, the sex drive may be heightened. Other women may feel nauseous or lightheaded.
- Check temperature. When an egg is released, progesterone levels go up, and this raises the body temperature slightly. A basal thermometer can be used to track the temperature, every morning before your partner gets out of bed.
- Use an ovulation kit. These convenient, highly accurate kits track hormone levels in the urine to determine when it’s the best time to try and start a family.
At the Center for Vasectomy Reversal, we love helping people start families with healthy pregnancies. We pride ourselves on helping men improve their fertility through uncompromising, concierge-level patient care. Under the direction of Dr. Joshua Green, our team provides state-of-the-art treatment for men who need a reversal of their vasectomy or have other fertility concerns. To learn more, contact us through our website or call 941-894-6428.
-
How Stress Affects Semen Quality

It’s long been understood that stress has an impact on a person’s health, so it comes as no surprise to learn that men’s reproductive health may be affected by stress. About 12 in every 100 couples in the United States struggles with infertility, and several studies over the past several years have established a link between poor semen quality and stress. Now, a new study is taking a closer look at both subjective and objective measures of stress to try to determine how it’s connected with semen concentration and sperm motility and appearance.
Male infertility is the problem for about 40 percent of couples with fertility issues. The main cause of male infertility is sperm abnormality, including misshapen or immobile sperm or low sperm production. Sometimes, these abnormalities are caused by medical conditions, but they can also be caused by health and lifestyle factors.
The new study, published in the journal Fertility and Sterility was conducted by researchers from the Rutgers School of Public Health in Piscataway, NJ and Columbia University’s Mailman School of Public Health in New York, NY. Between 2005 and 2008, researchers looked at 193 men between the ages of 38 to 49 who were a part of the Study of the Environment and Reproduction at the Kaiser Foundation Health Plan in Oakland, CA. The men completed a series of tests to measure stress levels, including workplace stress, stressful life events, and perceived stress. They also provided sperm samples, which were analyzed for semen concentration, sperm shape, and sperm movement (motility).
According to the researchers, men who felt stressed had lower concentrations of sperm and more sperm that were misshapen or had impaired motility. Even after considering other factors, like a history of reproductive health or other health problems, life stress negatively impacted sperm quality. Interestingly, job stress did not have the same effect. However, men with stressful jobs had lower levels of testosterone, and unemployed men had a lower quality of sperm than even stressed-out men with jobs.
The researchers don’t fully understand how stress affects semen quality, but they have some theories. It could be that stress triggers the release of glucocorticoids, steroid hormones which lower testosterone and dampen sperm production. Oxidative stress could also be a factor because oxidative stress in the body can degrade semen quality.
What is known is that a man can improve his fertility, even under stress, with healthy lifestyle habits. Staying physically active and practicing stress-reducing relaxation techniques can help, as can eating a nutritious diet and maintaining a healthy BMI. Men who are trying to improve their fertility should quit smoking, limit alcohol consumption, and talk to a doctor before beginning any new medication.
At the Center for Vasectomy Reversal, we pride ourselves on helping men improve their fertility through uncompromising, concierge-level patient care. Under the direction of Dr. Joshua Green, our team provides state-of-the-art treatment for men who need a reversal of their vasectomy or have other fertility concerns. To learn more, contact us through our website or call 941-894-6428.
-
How to Increase Male Fertility

If you and your partner are struggling to conceive a child, you’re not alone. About one in six couples struggles with infertility, and one in three cases is due to a problem with male fertility. There are some natural remedies you can try, though, that may boost your chances of conception.
- Load up your diet with healthy foods. Eat plenty of fruits and vegetables, focus on getting antioxidants and healthy fats. Limit your intake of saturated fats and red or processed meat. And be careful about eating soy, because it contains plant estrogen, which can reduce testosterone bonding and sperm production.
- Take your vitamins and minerals. Though the mechanism behind it is not completely understood, research indicates that vitamin D and calcium can impact sperm health. Vitamin C improves fertility by relieving oxidative stress in the body. Additionally, limited studies suggest folate and zinc can improve sperm concentration, count, and overall health.
- Quit smoking. Smoking is bad for every part of the body, so it should come as no surprise that it’s bad for your fertility. In fact, recent research indicates that smoking consistently reduces sperm count and people who smoked moderate or heavy amounts of tobacco had lower sperm quality than non-smokers or even light smokers.
- Watch the alcohol and drugs. Don’t drink to excess, don’t do any illegal drugs, and be mindful of your prescriptions. Some antibiotics, anti-androgens, anti-inflammatories, antipsychotics, opiates, antidepressants, anabolic steroids, supplementary testosterone, and methadone can all negatively affect your fertility. If you’re concerned about a medication you’re taking, talk to your doctor.
- Keep your cool. High temperatures can damage sperm, so if you’re trying to conceive don’t hold your laptop in your lap, wear tight underwear, or soak in hot tubs. Prolonged sitting and using car seat heaters can also cause overheating.
- Consider a supplement. Certain herbal supplements may be beneficial to fertility, including fenugreek, maca root, tribulus terrestris, and Indian ginseng. D-aspartic acid, a type of amino acid, may also be helpful.
- Reduce your exposure to environmental contaminants. Poor air quality and environmental toxins have been shown to decrease male fertility. Additionally, men in jobs with exposure to chemicals and overheating, like farmers, painters, varnishers, metalworkers, and welders, had higher incidences of infertility than other groups.
- Manage your stress. Stress raises cortisol levels, and cortisol lowers testosterone.
- Get some exercise and some sleep. For each, the key is to get just the right amount- not too little and not too much. Getting enough exercise and enough rest can improve your sperm count. It can also help you lose weight, which can improve your fertility.
If you’re struggling with infertility, call the Center for Vasectomy Reversal, where we love helping people build their families! We pride ourselves on providing optimal surgical results and uncompromising, concierge-level patient care. Under the direction of Dr. Joshua Green, our team provides state-of-the-art treatment for men who need a reversal of their vasectomy or have other fertility concerns. To learn more, call 941-894-6428 or contact us through our website.
-
Why your Libido May Be Lower than Normal

Is your libido lacking? Ebb and flow in sexual appetite is normal, but if you notice that your libido remains low for an extended time, it may indicate an underlying health issue. Let’s look at some causes of a low sex drive as well as possible treatments.
- Low testosterone is a common cause of a low sex drive. This makes sense because testosterone is an important male hormone. It’s responsible for building muscles and bone mass, stimulating sperm production, and boosting your libido. Normal testosterone levels vary, but a man is considered to have low testosterone when his level falls below 300 nanograms per deciliter. Talk to your doctor if you think this may be the case, because testosterone replacement therapy can help.
- Certain medications can knock you out of the mood. Blood pressure medications, chemotherapy or radiation, hormones used to treat prostate cancer, antidepressants, opioid pain relievers, corticosteroids, and even some heartburn and gastroesophageal reflux disease (GERD) medications can lower libido. If you think something you’re taking may be causing this issue, talk to your doctor about switching medications.
- Sleep problems can lead to libido problems. Restricted sleep, obstructive sleep apnea, and restless legs syndrome (RLS) can all play a part in lowering testosterone and, by extension, the sex drive. Research indicates that restricted sleep reduces the testosterone levels the next night. As to RLS, it can lead to erectile dysfunction and even impotency.
- Your mind has an impact on your sex drive. Depression can reduce your interest in sex, and this is further complicated by the fact that certain anti-depressants can also lower libido. Low self-esteem can also lead to anxiety about sexual performance, resulting in issues with ED or reduced sex drive.
- Chronic illnesses can make sex low on your list of priorities. Chronic pain, for instance, can drastically lower your libido. Illnesses like cancer can reduce your sperm production, and other conditions, like diabetes, obesity, high blood pressure, high cholesterol, and chronic heart, kidney, or liver failure can all take a toll. If you’re experiencing intimacy issues because of chronic illness, marriage counseling may help.
- Aging decreases testosterone. Testosterone levels are at their peak when men are in their late teens. The levels decrease as men age, but medication may help.
- Lifestyle habits may impact your libido. Heavy drinking can reduce the sex drive, as can illegal drugs. Even exercise can have a negative effect on your sex drive: too little or too much exercise can reduce libido. Stress, too, can decrease your sexual desire. Healthier lifestyle habits and stress management can help.
At the Center for Vasectomy Reversal, we pride ourselves on providing optimal surgical results and uncompromising, concierge-level patient care. Under the direction of Dr. Joshua Green, our team provides state-of-the-art treatment for men who need a reversal of their vasectomy or have other fertility concerns. To learn more, contact us through our website or call 941-894-6428 for a free consultation.
-
Vasectomy Reversal Myths

As you contemplate whether a vasectomy reversal is right for you, you may stumble upon common myths about this surgical procedure. Dispel any misunderstandings before you meet with a microsurgeon about reversing your vasectomy.
Myth: A vasectomy reversal is as straightforward as a vasectomy.
Almost any doctor can perform a vasectomy, a short and relatively simple surgery that requires minimal training. However, a correctly performed vasectomy reversal is an advanced, technically challenging microsurgery lasting two to three hours. You should only trust an expert microsurgeon with years of successful reversals to increase the chance of success and lower the risk of complications.
Myth: All vasectomy reversals have the same chance of success.
Talk to your surgeon about what could affect the success of your surgery before deciding to have a vasectomy reversal. Factors may include:
- Sperm count and mobility
- Any development of anti-sperm antibodies
- Scar tissue following surgery
- Fertility of your female partner
- Length of time since your vasectomy
Myth: A vasectomy reversal must be performed within 10 years to have any chance of success.
If you had your vasectomy less than five years ago, there is a greater than 95 percent chance of sperm in the ejaculate. Surgeries performed five to 10 years ago have about a 90 percent chance, and if 10 or more years have elapsed, there’s an 80 to 90 percent chance. Experienced surgeons can perform successful reversals over 20 years after a vasectomy. (Note: pregnancy rates are lower than the percentages given here and depend on numerous factors.)
Myth: Pursuing IVF is better than having a vasectomy reversal.
While in vitro fertilization is a viable infertility treatment, it should not be your first choice. IVF costs three to five times more than vasectomy reversal surgery, and it comes with serious risks to the mother and baby—all with no guarantee of a successful pregnancy. With the costs, risks, and success rates in mind, a reversal with natural conception makes more sense for most couples.
Myth: Some vasectomy methods are not reversible.
It is extremely rare for a vasectomy to be performed in such a way that a microsurgeon cannot reverse it. The only time this can happen is if the original surgeon removes too much of the vas deferens, the tube that transports sperm from the testes to the urethra. In this case, there is nothing to reattach, and the reversal cannot be done. Again, this is very uncommon and can be ruled out prior to surgery via a physical exam.
Dr. Joshua Green of the Center for Vasectomy Reversal is a leader in microscopic infertility procedures. If you have decided to pursue parenthood, we can help. Dr. Green has completed hundreds of vasectomy reversal surgeries and takes great pride in his remarkable success rates. We’ll discuss your surgical options, costs, and the chance of success based on your specific situation. To learn more, please call our Sarasota, FL clinic at 941-894-6428 or schedule a free consultation online.
Recent Posts
Popular Posts
categories
- Uncategorized
- Sperm Retrieval
- vasectomy reversal
- Emergency
- Dr. Green
- sperm count
- fertility
- male infertility
- MESA
- medical care
- low sperm count
- IVF
- male fertility testing
- anesthesia
- pregnancy
- sperm aspiration
- semen analysis
- post-vasectomy pain syndrome
- infertility
- VE
- anti-sperm antibodies
- older dad
- general anesthesia
- gender reveal party
- post-operative infections
- baby name
- parent
- baby's first year
- fertilization process
- spinal anesthesia
- ACS Fellow
- nutrition tips
- concierge-level care
- fertility planning app
- azoospermia
- out-of-town patients
- V-V
- post-vasectomy reversal
- conceiving
- vasectomy
- vasoepididymostomy
- smoking
- sperm quality
- baby registry
- infographic
- surgical care
- surgical consultation process
- prostate cancer
- baby gender
- family time
- COVID
- Baby Shower
- Child Care
- Halloween Costume Ideas for Babies
- Halloween
- Halloween Safety Tips
- Celebrity Infertility Spotlight
- Postpartum
- testosterone
- Father's Day
- Father
- Men's Health
- Thanksgiving
- Pregnancy Announcement
- Parenting Tips
- Sperm
